Recently, I put steak sauce on my veggie burger. I don’t know if that’s normal, but at least it made something about the awkwardly textured meal seem familiar.
The truth is, I crave these bits of familiarity at mealtime. Even today I’m disappointed thinking back to October, because had I known then that that Steak ‘n Shake burger was going to be the last time I’d ever eat red meat, I would have appreciated it more. Maybe I would have even gone somewhere else and chosen a better cut.
However, thanks to the bite of a sneaky little lone star tick, my diet — and my life — have changed forever.
After months of recurring hives, headaches, wheezy mornings, difficulty breathing, and feeling “low energy,” a blood test diagnosed me with the mammalian meat allergy, or what’s colloquially known as the alpha-gal allergy (named for the Galactose-alpha-1,3-galactose antibody). Red meat, pork, game, and anything else coming from a mammal are officially off my plate.
Though the alpha-gal allergy was first reported in 2002, it wasn’t until about a decade later that the news media latched onto it. It was primarily located in the Southeast U.S. — Virginia, North Carolina, Tennessee — all places where this particular tick thrives. The number of diagnosed cases is spotty; it’s probably in the low thousands, but my allergist says she sees two new patients a week in my area of Virginia. Far from an official count, this map shows where patients have self-reported to an online database. Places as spread out as New York and Kansas are seeing multiple cases.
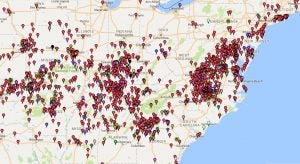
I can tell you, it sucks. I’ve never felt so knocked down in my life. Cross contamination is a daily threat. I spend as much time analyzing ingredient lists as I do walking from aisle to aisle in the grocery store. I keep an EpiPen close at hand and take over-the-counter allergy pills twice daily just in case.
The disease affects everyone differently, but the common thread is that if the meat comes from a mammal, we can’t eat it. Ever. And there is no cure. Symptoms, such as hives, usually develop three to six hours after contact with meat. That alone makes it hard to spot. It has often been misdiagnosed in patients, even in the areas where the ailment has long lived.
“This unusually long time gap between a meal and an allergic reaction is probably a big reason that alpha-gal allergies are often initially misdiagnosed,” said Dean Metcalfe, M.D., chief of the Mast Cell Biology Section in the Laboratory of Allergic Diseases in NIAID’s Division of Intramural Research. “If you start to have trouble breathing in the middle of the night, you probably are not going to blame the hamburger you had for dinner.”

A month after my diagnosis, the news got worse for me — dairy products were continuing to cause reactions, something that happens to only a small fraction of patients. So my cheese is now vegan (the varieties are limited, but the taste is decent compared to so many other vegan alternative foods out there) and my “milk” is plant-based. I tried various types of non-dairy “milk” and found only one that is passable. I’ve long not been a fan of chicken, so seafood and turkey are vital for protein. I’ve also, thankfully, discovered emu meat, which is delicious and comes closer than anything else to the taste of hamburgers and roasts of old.
This is my new normal. It’s one that has been hard at times to adapt to. I’ve encountered moments where I get immensely sad, somehow feeling that living in a rural area has turned against me. Sometimes, when breathing gets hard because of cross contamination or because I didn’t notice that Ingredient #20 on the package was beef fat, fear takes over. From college to marriage to career, I’ve often made choices that will direct and define the rest of my life, but they were just that: choices. The alpha-gal allergy was thrust upon me, with no say on my end. That’s what’s new for me; it’s what has made it particularly difficult.
I am lucky to have a supportive family and a deep faith, and there’s a strong social network of others who have alpha-gal. I also try to think of the fact that, in life as a whole, I’m luckier than many others out there. With extra care and adjusting habits, it’s manageable. Not everyone is given that opportunity in life.
This is my new normal. It’s one that has been hard at times to adapt to.
Being so entwined in agriculture, I’ve also wondered how this could affect the industry. Not only could farmers contract this disease, but if enough of the public gets it (and we’re talking a drastic increase), would we begin to see more livestock meat being used for exports rather than domestically — simple supply and demand at play?
Jason Carter, Executive Director of the Virginia Cattlemen’s Association, says that the allergy isn’t something that has impacted meat production to date. But he notes that it is something that has awareness in the beef industry.
“This disease acts like a chronic condition in that it changes the way in which your body metabolizes the unique sugars that are on the surfaces of mammalian red meat — it becomes, from a research standpoint, more like heart disease,” Carter said. “It doesn’t arrive in the way people usually think of chronic diseases, but long-term it doesn’t act in a way that it can be treated and goes away like an acute bacterial infection or something similar.”
As this takes hold in more areas of the nation, particularly seeping into the ag-heavy Heartland, be careful in your pastures and fields. One little bite can change everything.
Ryan Tipps is the managing editor for AGDAILY. He has covered farming since 2011, and his writing has been honored by state- and national-level agricultural organizations.



